Breast Reconstruction in Denver, CO
What is Breast Reconstruction?
Breast reconstruction restores a more natural, symmetrical appearance to the bosom, maintains body proportion, allows clothes to fit better, and most important of all boosts self-confidence for women who have lost one or both breasts to mastectomy or who lack breasts due to a congenital or developmental abnormality. Reconstructive surgeons strive to create a new breast and nipple that resemble a woman's natural breast as closely as possible in shape, size, and position.
Who is an ideal candidate for breast reconstruction?
Women whose cancer seems to have been cured with mastectomy are the best candidates for breast reconstruction. Those with significant health problems and those who smoke and are unable to quit, are advised to wait. But the majority of women choose reconstruction and choose immediate reconstruction, which means the reconstructive process begins at the time of the mastectomy. Delayed reconstruction means the reconstructive process begins many months after the mastectomy.
The reconstruction itself consists of multiple operations, the first of which involves the creation of the breast mound and is performed during or after mastectomy in a hospital under general anesthesia. Later surgeries, if necessary, may be done in the hospital or an outpatient facility, with either general or IV sedation anesthesia.
There are several ways to reconstruct the breast, both with and without implants. Dr. Bershof's practice encompasses implant reconstruction only but below will briefly discuss other options.
How is breast reconstruction performed?
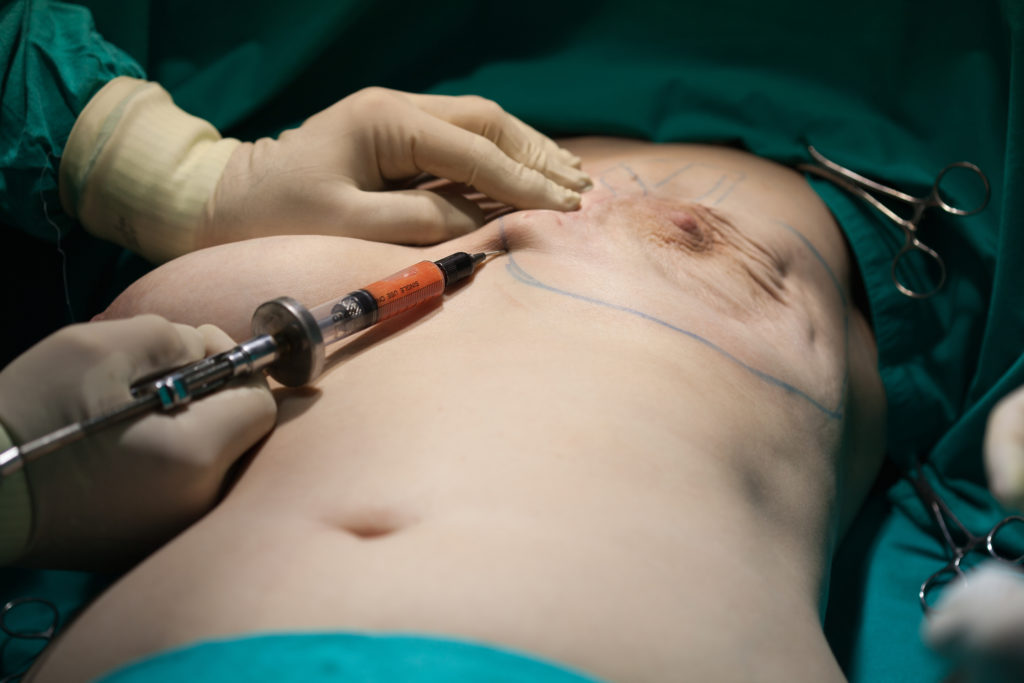
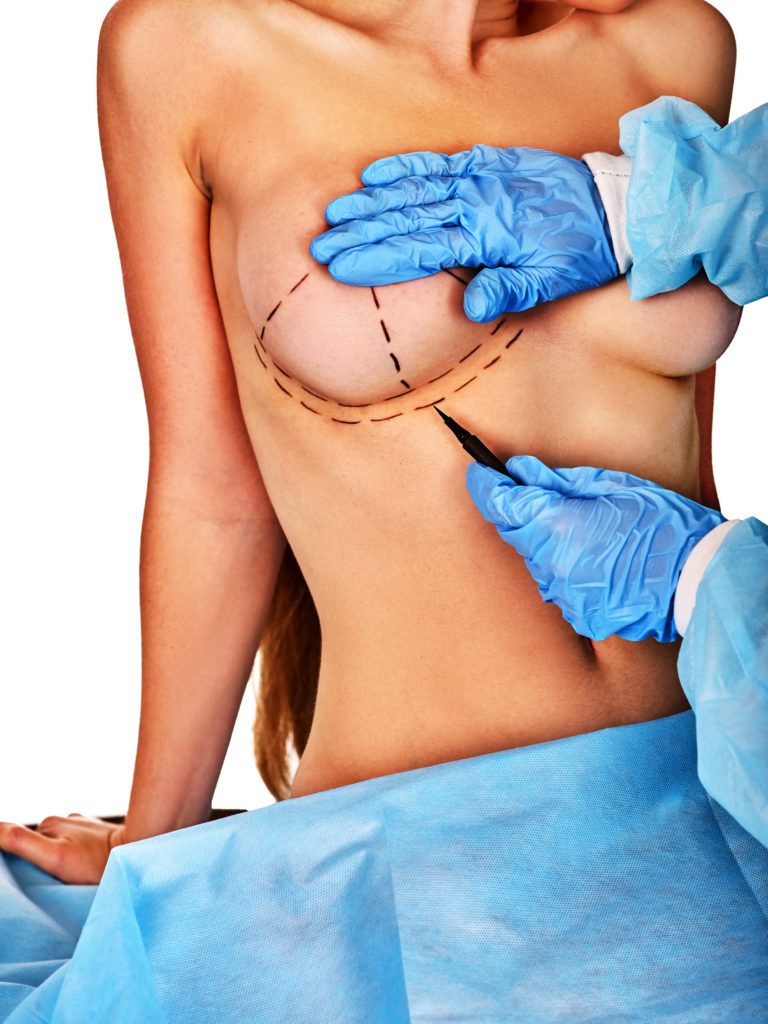
The most common technique, which Dr. Bershof performs, combines skin and muscle expansion with implant insertion. First, at the time of the mastectomy, a tissue expander is placed beneath the skin and chest muscle (pec muscle) where the reconstructed breast will be located. Beginning about one month after the mastectomy and placement of the expander, in the office, the saline (sterile saltwater) solution is then injected into the expander port beneath the skin and muscle. This expansion takes place every several weeks until the desired size is achieved, stretching the skin and muscle. After the last expansion, the stretched skin and muscle are allowed to recover for several more months and then at a second procedure, under general anesthesia, the expander is removed, the pocket adjusted for symmetry, and a semi-permanent implant placed (either saline or silicone gel). If both breasts are being reconstructed, they are matched as best as possible to each other. If only one breast is being reconstructed, it might be recommended at this 2nd procedure that the other breast undergo a symmetry procedure, such as an augmentation, breast lift, or breast reduction A final procedure reconstructs the nipple and areola (dark area of skin around the nipple).
Although Dr. Bershof only performs the above expander/implant technique, several of his colleagues perform what is called flap procedures, using tissue from other parts of the body to assist in building a breast mound. These procedures might still require an implant under the flap, such as the latissimus muscle flap, or not require an implant, such as a TRAM flap, free TRAM flap, or a DIEP flap. It is debatable if flap reconstructions look or feel better than implant techniques but certainly the pros and cons need to be weighed by the patient.
In either case, the reconstructed breast will probably look and feel different from the natural breast, maybe look and feel better, maybe not. This surgery is designed to make women who have undergone mastectomy, feel better in clothes and feel symmetric. After a mastectomy, the sensual sensation to the breast which courses through the nipple is lost; but the tactile sensation slowly recovers, albeit not completely, over 1-2 years.
Recovery after breast reconstruction
Recovery varies depending upon the surgery. The expander technique recovers sooner than the flap techniques. Most patients are able to return to office-type work 2 weeks, more or less, after mastectomy and expander placement; perhaps longer with flap techniques. Surgical drains at the time of the mastectomy and stitches are removed at about one week.
The reconstructed breast will be numb following surgery, but it is possible that some sensation will return as time passes. Scars will fade, but not disappear. Implants should be replaced every 10 years or so, especially the silicone gel implants according to the FDA.
Patients who receive chemotherapy after mastectomy, begin their chemotherapy about one month after surgery, which corresponds to when the tissue expansion begins. Chemotherapy slows down the expansion process somewhat but does not significantly impact results. Patients who need to receive radiation therapy, generally receive radiation after the chemotherapy which is also after the expansions are complete. Radiation therapy slows down the reconstructive process but more importantly, negatively impacts the aesthetic results of the reconstruction. Radiated skin, fat, and muscle become more fibrotic (scarred) and never recover, making the radiated breast less ideal. If results in the setting of radiation are unacceptable, fall back reconstruction includes converting to one of the flap techniques.
Possible risks and complications of breast reconstruction
Breast reconstruction has not been proven to affect the recurrence of cancer or other diseases, chemotherapy or radiation treatment. With regards to radiation, implants do not affect radiation therapy to be given but radiation therapy does affect implants.
Nevertheless, in addition to the complications possible from any surgical procedure (bleeding, fluid collection, excessive scar tissue, or difficulties with anesthesia), there are some risks inherent in breast reconstruction, including infection around the implant, if an implant is used, and capsular contracture, when the scar (capsule) around the implant tightens, causing the breast to feel hard. Treatment for capsular contracture varies but usually requires removal of the scarred capsule and placing a new implant. Some patients may need time to come to terms emotionally with their new breasts.
Want to learn more?
For more information about The Plastic Surgery Group, please call us at 303.399.7662 or click here.